Rebekah is fearless. I know this, not just from the fact that she fights a mean game of dodgeball, but also because she is an infertility warrior.
Rebekah is here to #FlipTheScript for national infertility awareness week, here’s her story...

First of all, tell us a little bit about you and your partner….how did you meet?!!
Hi! I’m Rebekah, 32, an Aussie living in the USA!! My Hubby is Will, we seriously have the most unconventional love story…it started as a nightmare. Christmas Eve 2014, I thought I would treat myself to a bathroom remodel. A few weeks later when the construction workers didn’t turn up to start their demolition work I called Will, the project manager from Home Depot overseeing my remodel. I was furious! Not one of my greatest moments, but let’s just say my vocab was very colorful. Six weeks later, two burst bathroom pipes, a leaky shower pan, new downstairs carpet, new ceiling drywall and paint, Will would manage to calm me down from this bathroom disaster every day. He became my new best friend.

When did you realize that you were facing a diagnosis of infertility, how did you find out and what were the issues that you faced?
In 2004 I went for my annual OBGYN checkup, I specifically remember the doc saying “oh, wow are you pregnant? Your uterus is quite large!!” Not something a single, 18 year old really expects to hear! I went for an ultrasound, and it seemed like the longest ultrasound of my life – I knew something was wrong. I was in there for two hours waiting for an explanation. It wasn’t until my follow up appointment that I found out that I had a 10cm x 8cm x 9cm mass on my left ovary.
I needed surgery. The first question I asked when I woke up from the procedure was “Is my ovary ok?” They told me they had to remove it. I was left in tears wondering what this meant for my future as a mother.
As well as losing my left ovary, I was diagnosed with Poly-Cystic Ovarian Syndrome (PCOS). I didn’t truly understand what PCOS meant until several years later when I was 22. I married young, and began my journey to have a baby. I was on Clomid and stimulants for almost a year, but the pressure of it all contributed to our break up. The stress of timed sex, and not knowing if I would get pregnant caused so much strain on our new marriage that it ended just 8 months after our wedding. For me, it was actually a blessing in disguise.
I suffered from endometriosis and over the years had several more surgeries to remove as much of it as possible, and then another two more surgeries on my right ovary for large cysts. Luckily, my one remaining ovary remained “safe.”
When I was 28 I started to panic, I lost 80lbs in order to try to preserve my eggies and one ovary from any more cysts. That was when I ventured to the fertility clinic specialist to get a baseline of where I was down below. I wanted to know what the future held and how I could become a mother.
Although I was single at the time, I realize now that I put too much pressure on myself . I wanted to be a mother so badly. The yearly surgeries took a toll on my body, and emotionally, I was a wreck. I thought that freezing my eggs would at least take some pressure off the fact that Mr. Right hadn’t come along yet, and give me the chance to be a mother.
My Reproductive Endocrinologist doctor was amazing; I didn’t get the news I wanted, but she reassured me about it all,: I had low AMH, low progesterone and estrogen, and with just one ovary, I was facing a lot of challenges. To add to it all, a Hysterosalpingogram (HSG) revealed a mass in my uterus and meant more surgery to remove.
By this point, Will and I had only been dating a month!! It felt weird to involve him so early, but I wanted to be transparent with him since not having children could be a deal breaker for some. Three months after my surgery to remove the uterine mass I went for a checkup…
…and there it was…the big 55mm cyst engulfing my ovary, my nightmares come true. The whole reason I was at this clinic was to be proactive in saving my ovary and getting eggs, and now it might not even happen – I was devastated.
I started hormonal treatment, but when I went in for a checkup we found it wasn’t working and the only choices was MORE surgery. But as I was prepped for surgery I finally got the good news I had been waiting for, the cyst had finally started to shrink! So the doc cancelled the surgery and when I went back for a follow up appointment, not only had the cyst continued to shrink, but I was about to ovulate! WHAT! I couldn’t even believe it!! And this was my opportunity!
I was faced with the ‘now-or-never question’…do I get a sperm donor? Do I see if my new-ish boyfriend of a few months is willing to do the deed??!
I took all the information I needed discussed it with Will, and well, he was 100% on board. I got pregnant that cycle with my now 2-year old son, Wyatt!
Where are you on your infertility journey now?
After I gave birth to Wyatt, I knew I wanted more children. I had a complicated pregnancy and birth, but we returned to the fertility clinic at 6 months post-partum to discuss number trying for number 2. But as I stopped breastfeeding I got pregnant, without intervention. Unfortunately that pregnancy ended in an interstitial pregnancy (this is a uterine, but ectopic pregnancy: the pregnancy is located outside the uterine cavity in that part of the fallopian tube that penetrates the muscular layer of the uterus.) I didn’t even know what an interstitial pregnancy was. I went for a D&C (Dilation & Curettage, a surgical procedure to remove the fetus) and also opted to take Methotrexate. This is a drug usually given to cancer patients, but as the pregnancy was in a challenging location the drug ensured that no more cells from the pregnancy would remain.
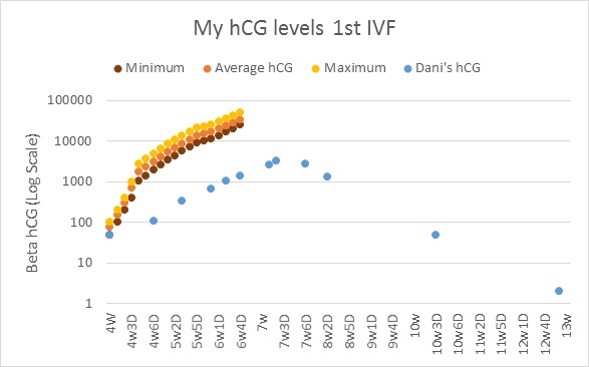
Two weeks after the treatment I began to experience severe pain on my left side (keep in mind I didn’t have a tube or ovary on the left). I discovered that my hCG beta levels were still rising, and not declining like the should have been; this meant that I was pregnant but they didn’t know where. I presented to the Emergency department with severe pain and they admitted me for pain management. Being that I work in healthcare I knew this was a “BS” diagnosis, they didn’t believe I was in pain and in their eyes had done everything- Ultrasound showed no internal bleeding, D&C and Methotrexate- what else could be done?
The doc told me “well I can take you to surgery but I’m going to pull your right ovary if we do.” My heart sank, I was in pain, but I did not want him to just pull my ovary because that would put me in to auto-menopause and shut down my baby factory. I went to bed to try and sleep off the pain. At 2 am I woke- I thought I was dying. I have never experienced pain like it in my life. I rang the buzzer and the nurse came. She was cold and heartless, standing at the door she told me “your Dilauded isn’t due for another hour.” I knew I didn’t need more pain meds, I needed a doctor, RIGHT NOW! The pain was like no other. 45 minutes of excruciating pain, I finally I found someone to help me as they walked past my room, they called rapid response, and within 10 minutes I was being prepped for the OR. My uterus had ruptured and I was bleeding internally. With my 6 month old baby and husband at home, I didn’t even know if I was going to see them when I woke up – not to mention having more children. I was terrified. Thankfully I am still here to tell my story. With another surgery under my belt, my journey just got even more complicated.
Four months post op I returned to the clinic to talk about trying to conceive #2… again!! I was scheduled for another HSG to check the integrity of my uterus after the surgery, but amazingly against all odds, I was actually pregnant with my now 7 month old daughter, Miss Emma.

Has infertility changed your relationship with your partner?
Will has been super supportive. But given he had “no issues” I always felt guilty for having all the doctors’ appointments, the bills and meds. I don’t think it really changed our relationship, but at times I did feel like I was a bit of a burden.
How has infertility impacted you financially? Did your healthcare insurance provide coverage for infertility treatment?
It makes me nervous to even think about how much we have spent between surgeries and medications! When I was on progesterone to support my three pregnancies, each time it was about $800/month. My insurance didn’t cover anything; and to date we have spent about $40k.
How have you taken care of yourself physically and emotionally during your struggles?
After my first miscarriage I ate my way through every emotion. At the time, it seemed like a great idea until I found myself weighing in at about 240lbs. I knew I would never get pregnant weighing that much with PCOS, so I lost 80lbs, it was life changing. Emotionally, I felt so much better, and physically I knew I was helping my body.
How have your friends and family supported you through your journey? Have you had any experience of lack of support or misunderstandings?
Looking back, I wish I had seen a counselor or therapist to help deal with my losses, but sadly I didn’t have much support from friends and family, I was left to cope on my own. The whole miscarriage topic is so taboo, I was scared to even bring it up, and felt like I just had to sweep it under the rug and move on.
Telling someone who just lost their baby or is trying to get pregnant that “it was meant to be”, “God has other plans” or “everything happens for a reason” did not help.
I had this longing for a baby and I couldn’t understand why this would happen, it was horrible. I wouldn’t wish any of this on anyone.
What has been the hardest point of your journey and how did you deal with it?
I think knowing that some things are just out of our control (as hard of a pill that is to swallow sometimes) taking things one day at a time, and just trusting the process helped me keep faith. Not giving up on my hopes of being a mother was my inspiration.
If you could go back in time, what advice would you give yourself?
I wish I had been gentler with my emotional health, and been more public about my journey. I am amazed at how many people have been through the same thing, and instead of hiding it and pretending like it isn’t an issue we should support each other.
As it’s national infertility awareness week, what message do you want to share about infertility to the general public?
The most difficult part about my journey was when people told me “don’t worry it will happen.” Thankfully my story did happen, but I have friends that haven’t had their sticky bean yet.
Is there anything else you would like to share that I haven’t asked you about?
While I was going through my journey I loved reading your blog, it gave me so much inspiration and peace knowing there are others out there that are also in a similar situation ❤
Rebekah, I think you have made me cry twenty times already. Through all your battles you have come out of the other side every time a true fighter. It might not have felt like it at the time, but I can see it from how you never really gave up.

Please leave a comment or message of support below for Rebekah and Will 🙂